Vestibular Rehabilitation Therapy (VRT)
This kind of rehabilitation therapy has demonstrated that vestibular disorders symptoms can be decreased. Symptoms such as vertigo, imbalance, dizziness, and/or visual disturbance can be found in patients with this kind of disorders. Secondary symptoms of nausea and vomiting, fatigue, reduced ability to concentrate or focus can also exist. The symptomatology can impact severely in the quality of life and day to day living of the patient. Social, emotional, familiar and work problems may appear due to this. Depression or a sedentary style of life can be seen in many patients, leading to other systemic medical conditions.
With this rehabilitation, those symptoms can be diminished allowing the patients to return to the normal lifestyle they had before.
What is vestibular rehabilitation therapy (VRT)?
Is a specialized form of therapy whose objective is to reduce primary and secondary symptomatology produced by vestibular disorders. It is based on a series of exercises designed to minimize vertigo and dizziness, lack of stability and/or imbalance. In many cases, the amount of vestibular restoration is minimum due to the level of damage to the system. However, these patients can feel better thanks to compensation exercises, which are based on the use of other senses like vision, touch, etc., substituting the damaged vestibular system. Nonetheless, parts of the nervous system like the cerebellum, vision and somatosensory sensations must be healthy so that the compensation may work.
In many cases, the process of compensation occurs in a natural way over time, but other patients with persistence of symptomatology need the help of vestibular rehabilitation therapy to promote compensation.
The good thing that VRT has is that it takes each person´s specific problem or problems into consideration to customize compensation exercises. Therefore, before starting the rehabilitation sessions, patients must undergo a full clinical examination and specialized tests. Depending on the identified vestibular problems, the patient may need Habituation, Gaze Stabilization and/or Balance Training.
Exercises to reduce symptoms
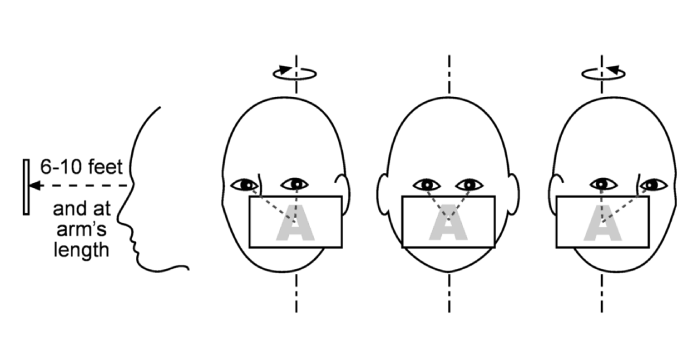
Habituation exercises are used to diminish dizziness produced by self-motion and/or visual stimulation. This kind of exercises are indicated for patients with dizziness that increases during quick head movements, positions changes of the head, among other head position changes, and during rapid visual stimulation such as going to shopping malls, watching a movie, walking over a shiny floor, etc. However, these exercises are not appropriate for patients with dizziness produced spontaneously and which does not get worst with head movements or visual stimulation. Habituation therapy reduces dizziness symptoms by exposing the patient repeatedly to specific movements or visual stimuli that provoke symptomatology. The dizziness level may increase, but should be only temporary and, before continuing with other exercises, dizziness level should decrease. With time and perseverance, dizziness levels will decrease to a minimum thanks to brain habituation.
Gaze Stabilization exercises are based on the improvement of eye movements during head movement to have a better vision. These are particularly appropriate for patients that have visual problems when reading, identifying objects of the environment, especially while they are moving. There are two types of gaze stability exercises. One is based on the fixation of eyes on an object while they repeatedly move their heads in multiple directions for a few minutes. The other type is based on using vision and somatosensation as substitutes for the damaged vestibular system. These are especially indicated to patients with vestibular function severely damaged.
Balance Training exercises are based on the improvement of steadiness to deal in a better way daily activities. These exercises should be patient specifics according to the type of vestibular disorder and balance problem that they have. The exercise needs to be challenging but safe. Among the exercises, patients may do: visual and/or somatosensory cues, dynamic and coordinated movements, stationary positions, and/or doing a task while balancing. These exercises should help the patient improving his ability to walk outside on irregular ground or in the dark. Walking, standing, bending, turning, reaching, running may be improved after these exercises.
VRT exercises are not difficult, but to achieve maximum success, the patient must be involved and committed to them. At first, symptoms may get worse, but with perseverance and consistency, patients will get better. Daily exercises will increase chances of improvement. Alongside the rehabilitation therapy, medical personnel will educate patients to help them understand their vestibular disorder and symptomatology, and the rehabilitation process that they are fulfilling.
Factors that can impact recovery:
Obviously, the vestibular disorder of every patient can affect recovery. Stable vestibular disorders (labyrinthitis) have better chances of improving than progressive vestibular disorders (multiple sclerosis, Meniere´s disease). Behavioral changes, the use of medication, physical therapy and/or surgical intervention can increase rehabilitation therapy success. Bilateral lesions (both ears) have fewer chances of recovery than patients with unilateral lesions. Nervous system lesions limit the amount and speed of recovery.
As said before, a sedentary lifestyle produced by minimizing dizziness symptoms triggers can cause secondary problems that slowly will affect vestibular rehabilitation therapy. Pain and medical conditions contribute to lack of balance and may increase the risk of falls. Also, patients tend to restrict their movements and rehabilitation exercises leading to a sedentary lifestyle. Certain medication can cause side effects similar to the one produced by the vestibular disorder, which magnifies the existing problems. Clinical personal must decide if the use of medication is necessary, taking in consideration patient´s symptomatology and priorities. If prescribed, physicians must control the correct usage of medication to achieve better results. Emotional concerns can diminish rehabilitation therapy success, so the need for psychological counseling may be necessary to help the patient.
Can dizziness symptoms return after disappearing?
Unfortunately, yes they can. Decompensation may occur in patients with permanent vestibular system damage due to different stressors (emotional and/or physical). Returning to the exercises that promoted previous compensation can help once again to achieve recovery. Usually, recovery of the decompensation is faster than previous compensation. It is important for patients to have regular consultations with their physician to make sure nothing new has happened.